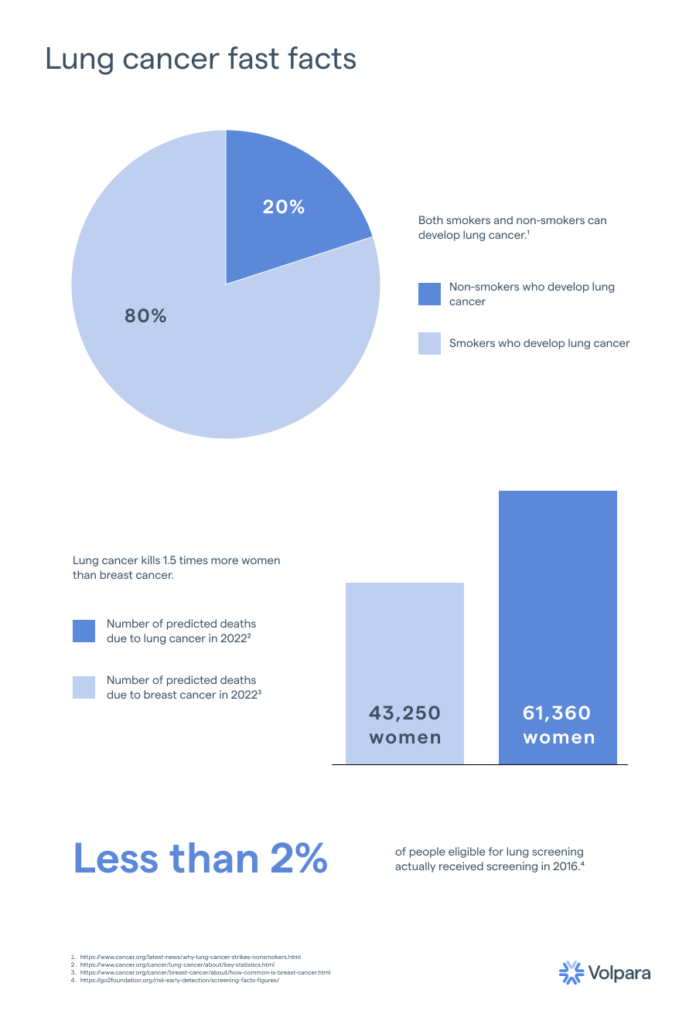
Lung cancer is the number one cancer killer in the United States for both men and women. In fact, lung cancer kills approximately 50% more women than breast cancer,1 and in many cases, these women were not smokers. In the same way that many women believe they are not at risk for breast cancer if they have no family history of the disease, many people think that lung cancer awareness is only applicable for cigarette smokers. These are both dangerous misconceptions—85% of women who develop breast cancer have no known family history of the disease2 and nearly 20% of patients who develop lung cancer have never smoked a cigarette.3 It’s time to make lung health a priority for all patients.
What does prioritizing lung health look like? The first step is to improve screening rates: In 2016, less than 2% of people eligible for lung screening actually received screening, despite lung cancer contributing to a higher rate of annual patient mortality than the next three most deadly cancers combined (colorectal, breast, and prostate cancer).4,5 But lung cancer doesn’t need to be so deadly—low-dose CT (LDCT) scans make it possible to detect lung cancer early—before symptoms occur, when it is most treatable and even curable.6 In fact, LDCT is currently the only method proven to do so.7
It is important to detect lung cancer early, before it spreads outside of the patient’s lung. Cancer that has not spread outside the lung is considered a stage one cancer and has a 63% five-year survival rate for non-small cell lung cancer.8 This is compared to a 35% five-year survival rate for cancer of the same type that has spread immediately outside of the lung (regional lung cancer), and a 7% five-year survival rate for cancer of the same type that has spread to more distant parts of the patient’s body (distant lung cancer).8 These statistics indicate a huge increase in patient survival with early cancer detection, and yet only about 16% of lung cancers are diagnosed at stage one due to the low screening rate.9
While all patients should invest in their lung health, it’s especially key to understand which patients are at higher risk of developing lung cancer and what is recommended for those high-risk patients. Current guidelines from the United States Preventative Services Task Force (USPSTF)10 identify high-risk patients as those who:
- Are between 50 and 80 years of age.
- Currently smoke or have quit smoking within the past 15 years.
- Have a 20 pack-year smoking history. (Pack years are calculated by multiplying the number of cigarette packs a patient smokes per day by the number of years they smoked daily.)
These guidelines have recently been expanded, meaning that patients that may not have qualified as high-risk two years ago are now considered at high-risk of developing lung cancer. High-risk patients are recommended to receive annual low-dose CT scans—it is essential to inform these patients about their need to start regular lung screening immediately if we hope to increase the survival rate of lung cancer patients. In fact, educating patients and evaluating their lung cancer risk during their annual mammogram appointments has shown potential to increase screening rates and save lives.11
Furthermore, the Centers for Medicare & Medicaid Services (CMS) has proposed changing the reimbursement for lung cancer screening such that it will match the updated USPSTF guidelines, giving lung screening centers more revenue stream.
Our mission at Volpara Health is to save more families from cancer. To learn more about how Volpara Lung may be able to help your facility track and manage patients who are eligible for lung screening, contact us at info@volparahealth.com.
References:
1. https://www.lungevity.org/for-supporters-advocates/lung-cancer-awareness/lung-cancer-statistics
2.https://www.breastcancer.org/symptoms/understand_bc/statistics#:~:text=In%20men%2C%20BRCA2%20mutations%20are,family%20history%20of%20breast%20cancer.
3. https://www.cancer.org/latest-news/why-lung-cancer-strikes-nonsmokers.html
4. https://go2foundation.org/risk-early-detection/screening-facts-figures/
5. https://www.cancer.org/cancer/lung-cancer/about/key-statistics.html
6. https://www.uofmhealth.org/health-library/abr9976
7. https://go2foundation.org/risk-early-detection/about-screening/
8. https://www.cancer.org/cancer/lung-cancer/detection-diagnosis-staging/survival-rates.html
9. https://www.lung.org/lung-health-diseases/lung-disease-lookup/lung-cancer/resource-library/lung-cancer-fact-sheet
10. https://www.uspreventiveservicestaskforce.org/uspstf/recommendation/lung-cancer-screening
11. https://pubmed.ncbi.nlm.nih.gov/33947284/

